
It is now obvious to observe that the COVID-19 pandemic has manifested a sweeping, future-oriented zeitgeist that has deep implications for every aspect of the way we manage our affairs. The coronavirus has, in turn, inspired a mood of divergent speculation regarding the broad impact of the crisis, which has been especially consequential for the professional and academic design, architecture, urban planning and public health fields. On the table is a sprawling range of interrelated topical themes belonging to those disciplines: the essential vitality of urban environments; the compromised case for urban density; the retrenchment of globalization; the future of commercial office spaces and remote work; the reversal of secular trends driving de-suburbanization; equitable affordable housing solutions; the role of climate change in infectious disease resilience; the relationship between pandemic health risk and structural discrimination; the development of biologically-inspired medical equipment; the role of private universities during national crises; and the renewed interest in infectious disease mitigation for building regulation.

Aside from a diverse chorus of reactions to the specter of paralyzing pandemic crises and their wide repercussions, in various cases, professionals working in the design-related world took direct material action to stem the tide of the virus. In an exceptional example, since early March, an interdisciplinary cadre of hundreds of designers, technical experts and medical professionals from around the world—organized around the capacities of the Harvard University Graduate School of Design (GSD)—have assembled as a non-hierarchical design-implementation working group to develop and fabricate personal protective equipment (PPE) and patient isolation hoods (PIH) for frontline medical workers in response to COVID-19.
In an open-source collaboration largely conducted remotely over Slack channels, production efforts have involved weeks of coordination between academic and technical experts from GSD faculty and staff, as well as professionals from Harvard’s numerous schools and institutes, such as the Harvard T.H. Chan School of Public Health and the Wyss Institute for Biologically Inspired Engineering at Harvard Medical School. The design implementation process has also been organized in close coordination with various medical institutions in the Boston-area, such as Mass General’s Brigham’s Center for COVID Innovation (MGBCCI) and Brigham and Women’s Hospital (BWH). Harvard GSD’s Fabrication Lab—equipped with CNC routers, laser cutters, Zund cutters, 3-D scanners, and other state-of-the-art technology—has served as an informal operational headquarters throughout the process.
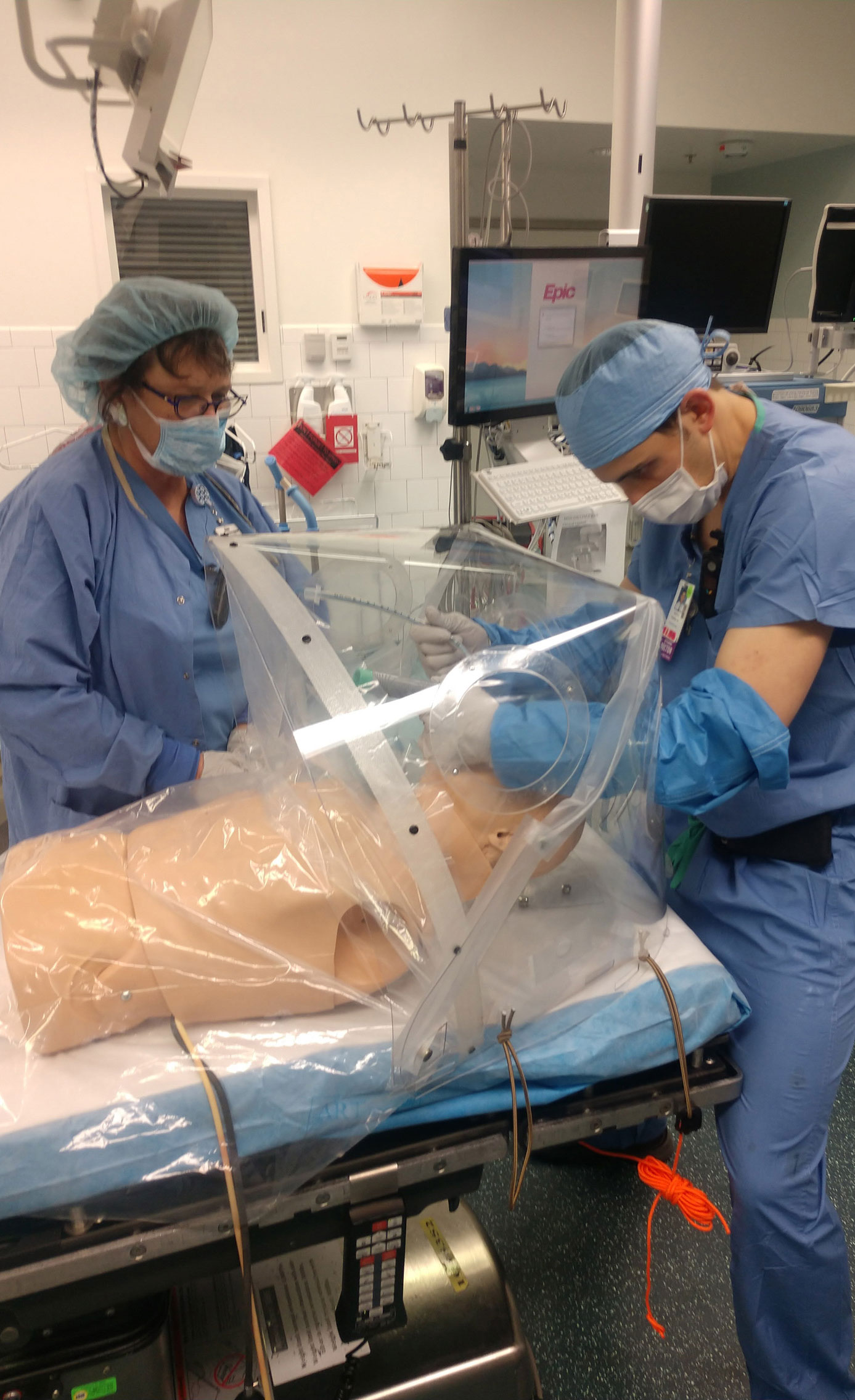
On the clinical side, Harvard GSD’s PIH efforts have been guided by Dr. Samuel Smith, MD, an anesthesiologist at Massachusetts General Hospital and instructor at Harvard Medical School, and Dr. Heung Bae Kim, MD, Director of Boston Children’s Hospital’s (BCH) Pediatric Transplant Center and Professor of Surgery at HMS. Design process has involved a range of engineers, architects, and fabricators, including members of the Harvard GSD architecture faculty and of Harvard's Wyss Institute. The novelty of this non-hierarchical and cross-institutional effort has quickly become a potential model for future pandemic responses, which may require rapid prototyping and fabrication of medical equipment for speedy deployment. As Dr. Smith observes in a press release published by the GSD on May 12, 2020: “the design process was unprecedented, partially because of the speed at which it was conducted, but also because of its ground-up, open-source, and collaborative design process.” Eric Höweler, an Associate Professor in Architecture at Harvard GSD, whose heavily involved in the design implementation process, further notes that “Fortunately, the maker movement has created a decentralized, rapid-prototyping network for small quantity production of components. Social networks were able to rally resources, and volunteers stepped up.”
Throughout March and April, the Harvard GSD—most specifically, its Fabrication Lab staff—produced thousands of 3-D-printed face shields and other personal protective equipment for Mass General Brigham. By May 7, the GSD had fabricated close to 3,200 face shields and 2,200 face visors. In addition to the fabrication of PPE equipment, at the end of March, the development of PIH equipment became a central focus of the collective working group. Doctors and clinicians identified twenty-five critical design requirements for the hoods, including easy access for doctors’ arms and medical tools, rapid retractability in case of emergency, and negative air pressure, or suction, to move contaminants and air particles away from the attending doctor.

After reviewing numerous PIH models, the team achieved consensus on one optimal design, dubbed “Apollo.” An “Apollo” prototype was delivered to Massachusetts General Hospital (MGH) on April 12 for clinical tests, after which it was approved for clinical use. The various PIH prototypes are designed to function across hospital settings, whether emergency room, intensive care unit, or otherwise, and to allow ease of assembly, use, and disposal; they are composed of flat sheets of polyethylene terephthalate glycol (PETG) plastic, and with minimal joinery and panel-construction needs. As an open-source design, the hoods can be fabricated anywhere in the world. “This is the first pandemic of the ‘jet age,’” Höweler distinguishes, “but it’s also the first pandemic of the ‘digital fabrication age,’ where expertise and open-source content moves freely, and individuals are networked for a common cause. It may turn out to be the thing that brings us together in different ways.”



